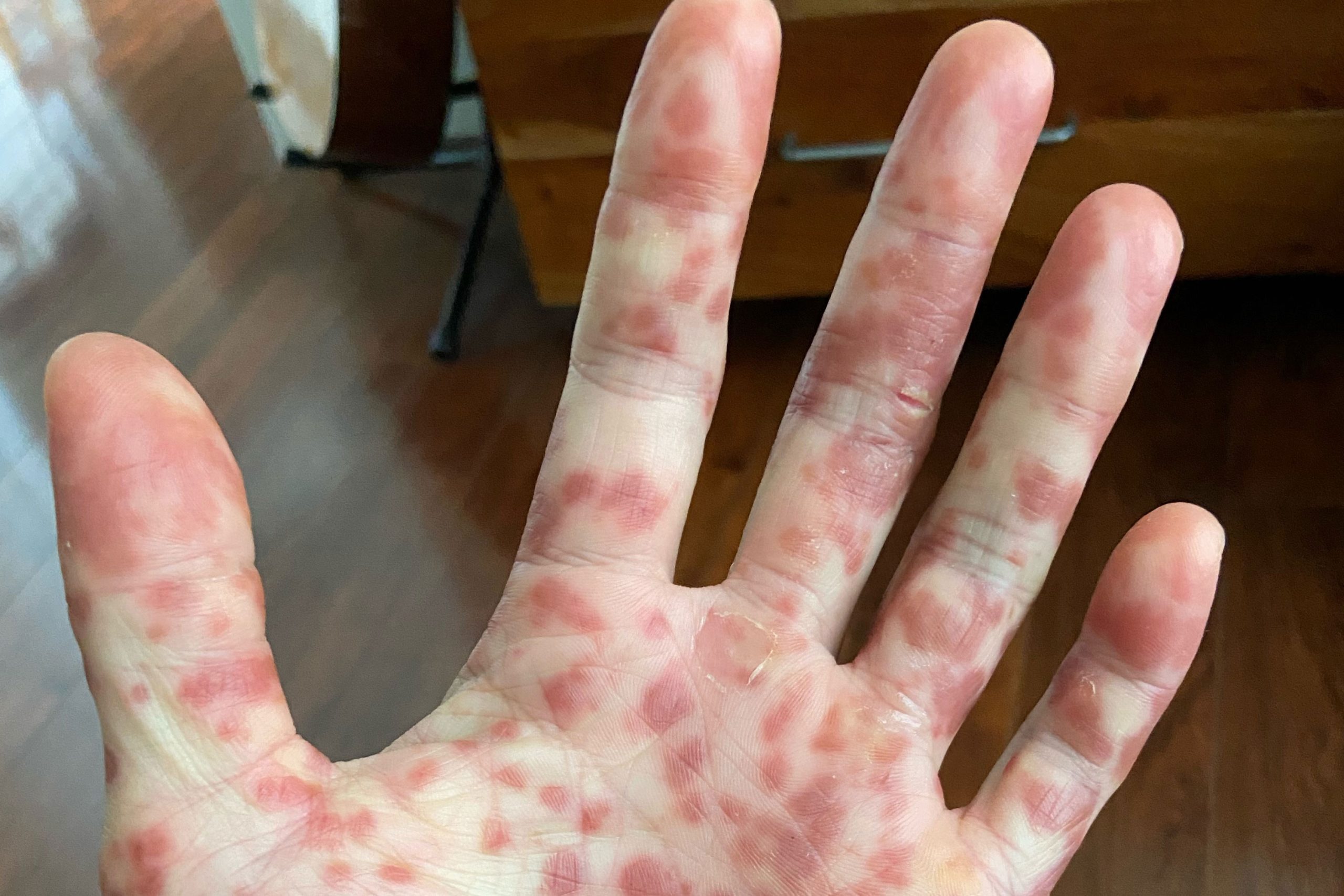
Two days after Kevin Kwong flew home to California from New York, his hands itched so badly, the pain jolted him from sleep. He thought the problem was eczema.
“Everything started rapidly getting worse,” the Emeryville, California, resident said. “I started to get more spots, on my face, more redness and they started leaking fluid. The rash expanded to my elbows and my hands and my ankles.”
It took Kwong, 33, six virtual appointments with doctors and nurses, one call to a nurse hotline, a trip to an urgent care clinic, two emergency room visits, and two incorrect diagnoses before an infectious disease specialist diagnosed him with monkeypox in early July.
Despite taking two tests, he never tested positive.
As the number of monkeypox cases has exploded in the U.S. in the past month, the public health system is struggling to spread the word about the virus’s danger and distribute a limited supply of vaccines to vulnerable people. But the problem extends even further. People who may be infected are grappling with dead ends, delays, incorrect diagnoses, and inappropriate treatments as they navigate an unprepared and ill-informed health care system.
The once-obscure virus has hospitals racing to teach emergency room staffers how to correctly identify and test for it. Dr. Peter Chin-Hong, the infectious disease specialist at the University of California-San Francisco who ultimately diagnosed Kwong, said his case was a tipping point for the research hospital.
“Kevin came in the middle of the night when a lot of resources weren’t available. So I think after his case, we’re doing a lot more education of the general condition. But I think your average clinician doesn’t always know what to do,” Chin-Hong said.
Monkey …