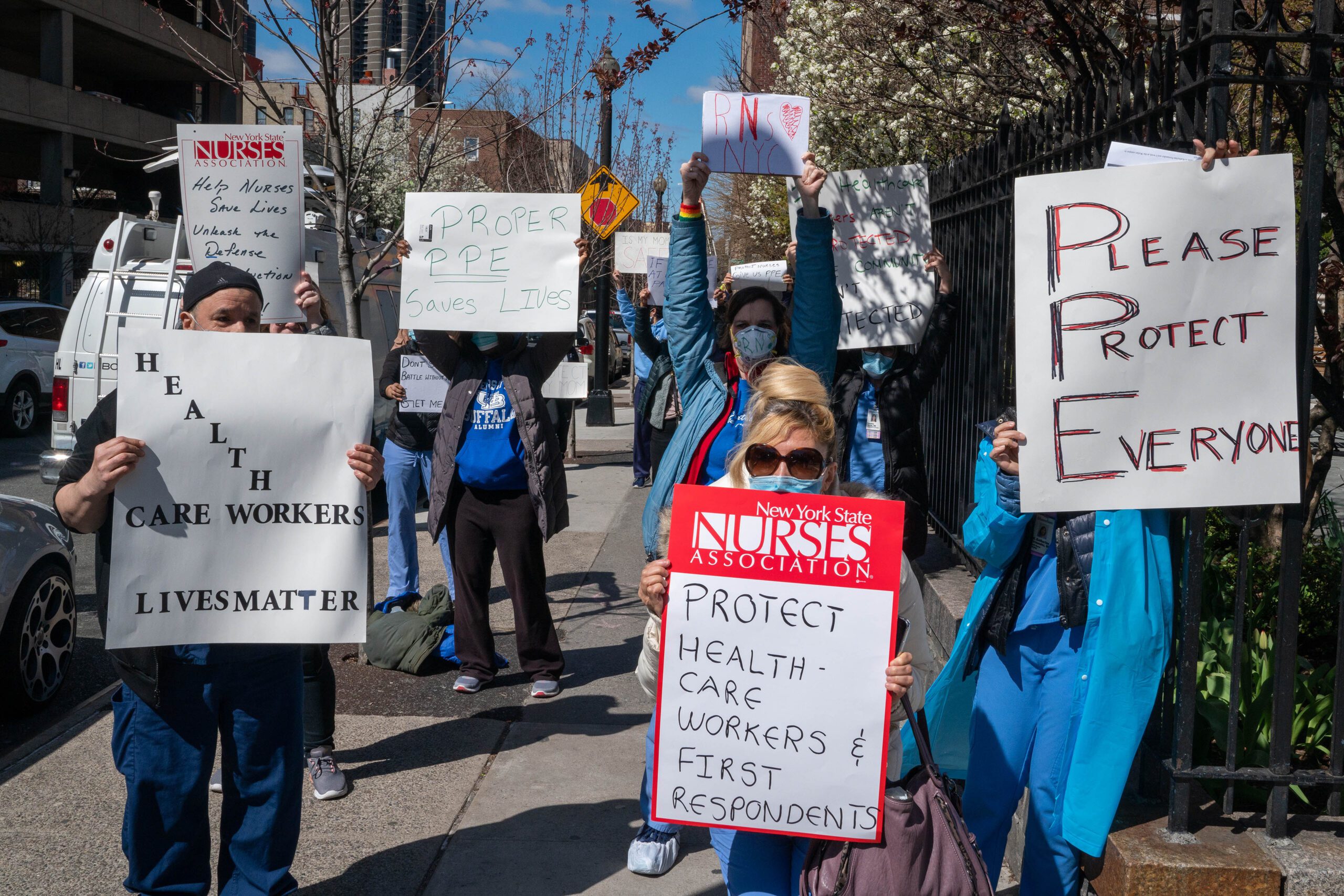Four years after hospitals in New York City overflowed with covid-19 patients, emergency physician Sonya Stokes remains shaken by how unprepared and misguided the American health system was.
Hospital leadership instructed health workers to forgo protective N95 masks in the early months of 2020, as covid cases mounted. “We were watching patients die,” Stokes said, “and being told we didn’t need a high level of protection from people who were not taking these risks.”
Droves of front-line workers fell sick as they tried to save lives without proper face masks and other protective measures. More than 3,600 died in the first year. “Nurses were going home to their elderly parents, transmitting covid to their families,” Stokes recalled. “It was awful.”
Across the country, hospital leadership cited advice from the Centers for Disease Control and Prevention on the limits of airborne transmission. The agency’s early statements backed employers’ insistence that N95 masks, or respirators, were needed only during certain medical procedures conducted at extremely close distances.
Such policies were at odds with doctors’ observations, and they conflicted with advice from scientists who study airborne viral transmission. Their research suggested that people could get covid after inhaling SARS-CoV-2 viruses suspended in teeny-tiny droplets in the air as infected patients breathed.
But this research was inconvenient at a time when N95s were in short supply and expensive.
Optical methods show how air flows between two men conversing. (Tang et al. / PLoS ONE)
Now, Stokes and many others worry that the CDC is repeating past mistakes as it develops a crucial set of guidelines that hospitals, nursing homes, prisons, and ot …
Article Attribution | Read More at Article Source
Four years after hospitals in New York City overflowed with covid-19 patients, emergency physician Sonya Stokes remains shaken by how unprepared and misguided the American health system was.
Hospital leadership instructed health workers to forgo protective N95 masks in the early months of 2020, as covid cases mounted. “We were watching patients die,” Stokes said, “and being told we didn’t need a high level of protection from people who were not taking these risks.”
Droves of front-line workers fell sick as they tried to save lives without proper face masks and other protective measures. More than 3,600 died in the first year. “Nurses were going home to their elderly parents, transmitting covid to their families,” Stokes recalled. “It was awful.”
Across the country, hospital leadership cited advice from the Centers for Disease Control and Prevention on the limits of airborne transmission. The agency’s early statements backed employers’ insistence that N95 masks, or respirators, were needed only during certain medical procedures conducted at extremely close distances.
Such policies were at odds with doctors’ observations, and they conflicted with advice from scientists who study airborne viral transmission. Their research suggested that people could get covid after inhaling SARS-CoV-2 viruses suspended in teeny-tiny droplets in the air as infected patients breathed.
But this research was inconvenient at a time when N95s were in short supply and expensive.
Optical methods show how air flows between two men conversing. (Tang et al. / PLoS ONE)
Now, Stokes and many others worry that the CDC is repeating past mistakes as it develops a crucial set of guidelines that hospitals, nursing homes, prisons, and ot …nnDiscussion:nn” ai_name=”RocketNews AI: ” start_sentence=”Can I tell you more about this article?” text_input_placeholder=”Type ‘Yes'”]